bowel obstruction / impaired intestinal transit disorders#
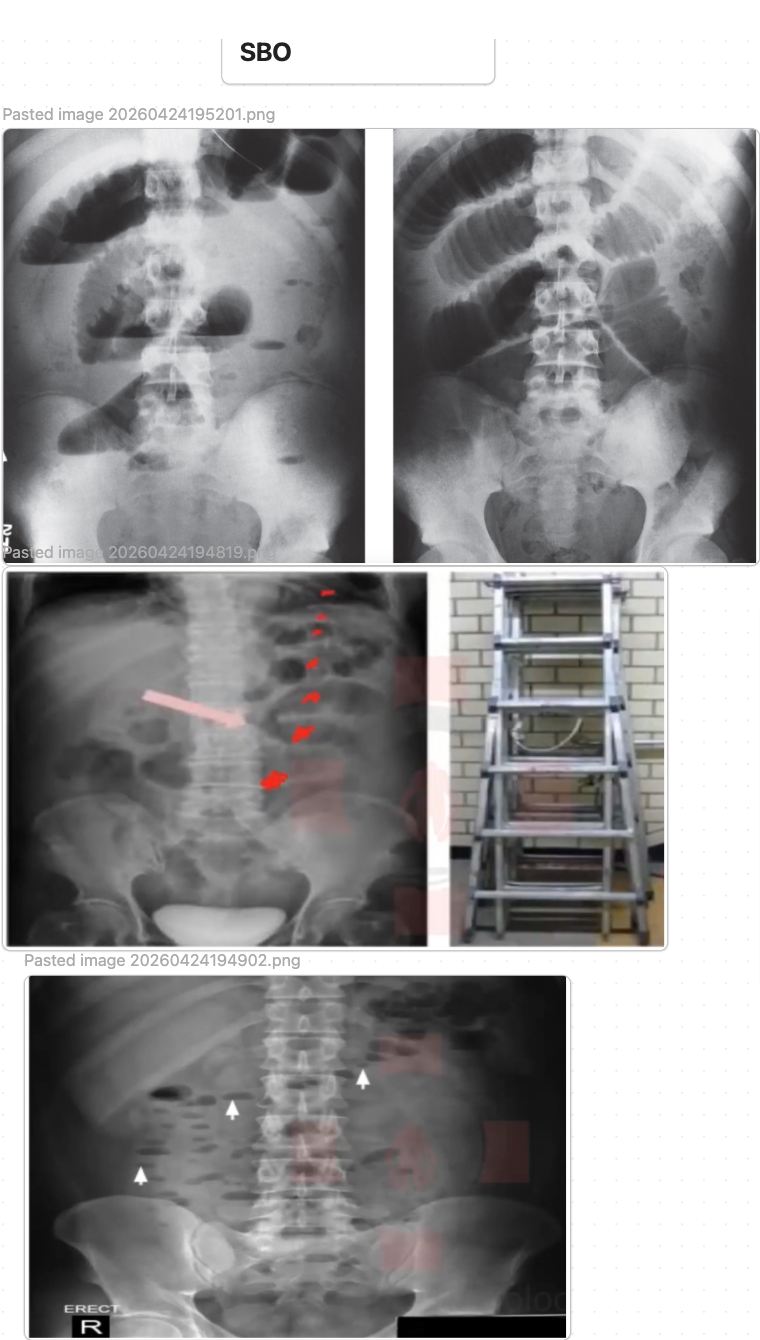
Small Bowel Obstruction (SBO)
Duration:
CC: abdominal pain, nausea/vomiting
Onset/Progression: s/g-w/i/u
PP: abdominal distension, constipation, last BM? flatus.?
PN:denies hematemesis, melena/BRBPR, fever/chills, dysuria, chest pain/SOB
mHx: prior abdominal surgery (adhesions), hernia, malignancy, IBD/Crohn’s, prior SBO, radiation, chronic constipation, opioid use.
sHx: tobacco, EtOH, drug use
initial DATA: CBC, CMP/BMP, Mg/Phos, lactate; KUB may show dilated central small-bowel loops (>3 cm) with air-fluid levels and little distal colonic/rectal gas. CT A/P w contrast is usually obtained if SBO suspected and may show dilated small-bowel loops to a transition point with air-fluid levels and possible complications such as ischemia or closed-loop obstruction.
pending DATA:
MEDS:
DDX: LBO, Ileus
COURSE:
PE: distended/tender abdomen, high-pitched bowel sounds or absent sounds
Plan
General Surgery consult early (if unstable urgent consultation)
Unstable, peritonitic, ischemic, or perforated = urgent surgery.
NG tube to low intermittent suction if vomiting, significant distension, pain
NPO (bowel rest)
IV fluids (LR/NS) + correct dehydration
daily labs for Electrolyte repletion (K, Mg, Phos)
Antiemetics (Ondansetron)
Pain control APAP (avoid excessive opioids if possible)
Serial abdominal exams
Monitor vitals, urine output, labs (CBC, BMP, lactate)
PT/OT for eval when stable
Urgent surgery if peritonitis, strangulation/ischemia, closed-loop obstruction, perforation, incarcerated hernia, worsening sepsis/rising lactate, or failure of conservative management.
bowel obstruction / impaired intestinal transit disorders
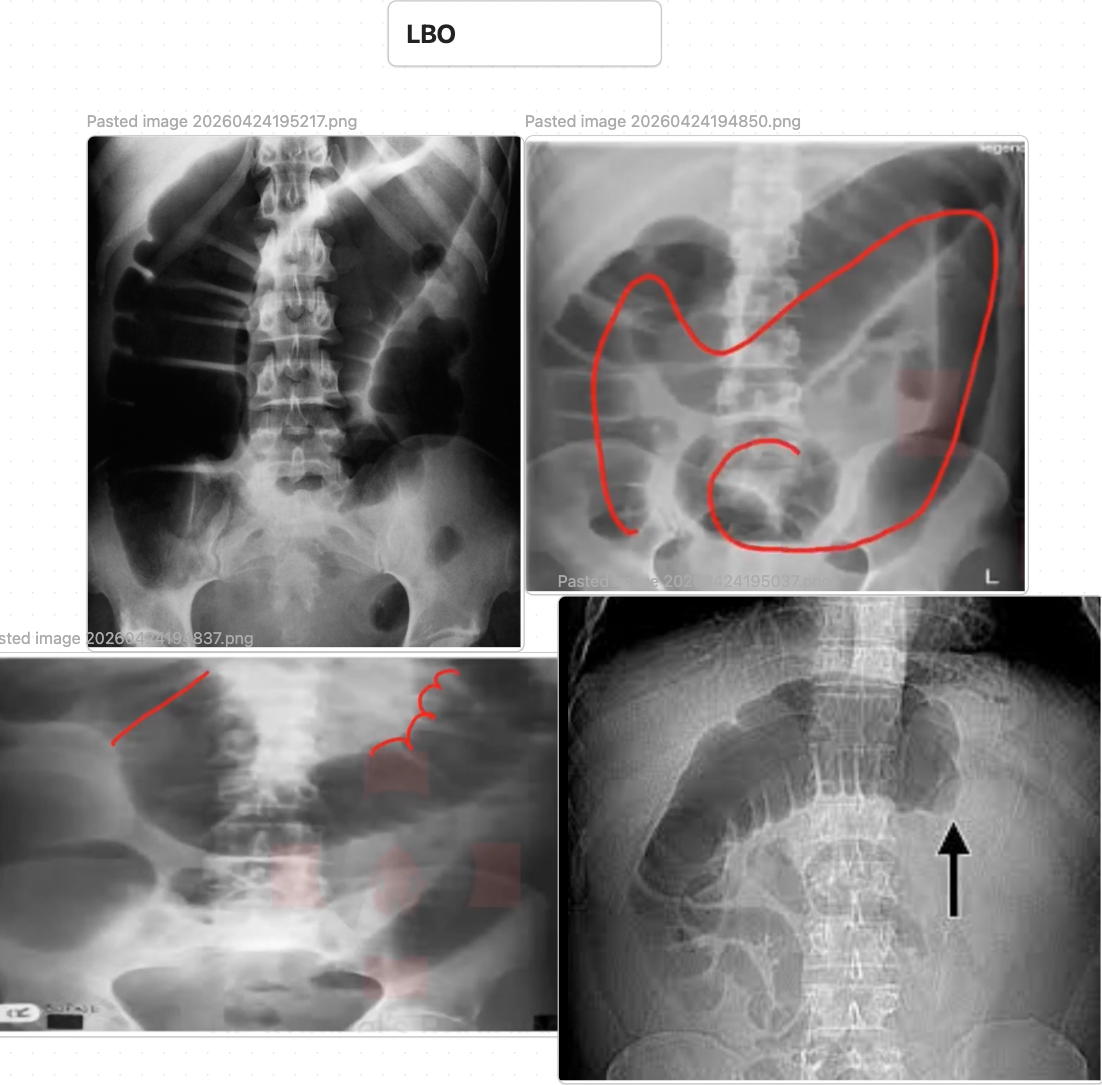
Large Bowel Obstruction (SBO)
Duration:
CC: abdominal pain, nausea/vomiting, constipation/obstipation
Onset/Progression: s/g-w/i/u
PP: abdominal distension, constipation, last BM? flatus.?
PN:denies hematemesis, melena/BRBPR, fever/chills, dysuria, chest pain/SOB
mHx: colon cancer/polyps, prior abdominal surgery, diverticulitis/stricture, volvulus history, IBD, chronic constipation, neurologic disease, opioid use.
sHx: tobacco, EtOH, drug use
initial DATA: CBC, CMP/BMP, Mg/Phos, lactate; KUB may show dilated peripheral colonic loops proximal to obstruction with paucity of distal rectal gas, ± coffee-bean sign if volvulus. CT A/P w contrast is usually obtained if LBO suspected and may show dilated colon to a transition point with distal decompression, possible cause (mass/stricture/volvulus), and complications such as ischemia or perforation.
pending DATA:
MEDS:
DDX: SBO, Ileus
COURSE:
PE: istended abdomen, tenderness, high-pitched or decreased bowel sounds,
Plan
General Surgery consult early (if unstable urgent consultation)
Unstable, peritonitic, ischemic, or perforated = urgent surgery.
NG tube to low intermittent suction if vomiting, significant distension, pain
NPO / bowel rest (oral bowel prep contraindicated)
IV fluids (LR/NS) + correct dehydration
daily labs for Electrolyte repletion (K, Mg, Phos)
Antiemetics (Ondansetron)
Pain control APAP (avoid excessive opioids if possible)
Serial abdominal exams
Monitor vitals, urine output, labs (CBC, BMP, lactate)
PT/OT for eval when stable
Urgent surgery if peritonitis, strangulation/ischemia, closed-loop obstruction, perforation, incarcerated hernia, worsening sepsis/rising lactate, or failure of conservative management.
Broad-spectrum antibiotics if concern for ischemia, perforation, or sepsis
bowel obstruction / impaired intestinal transit disorders
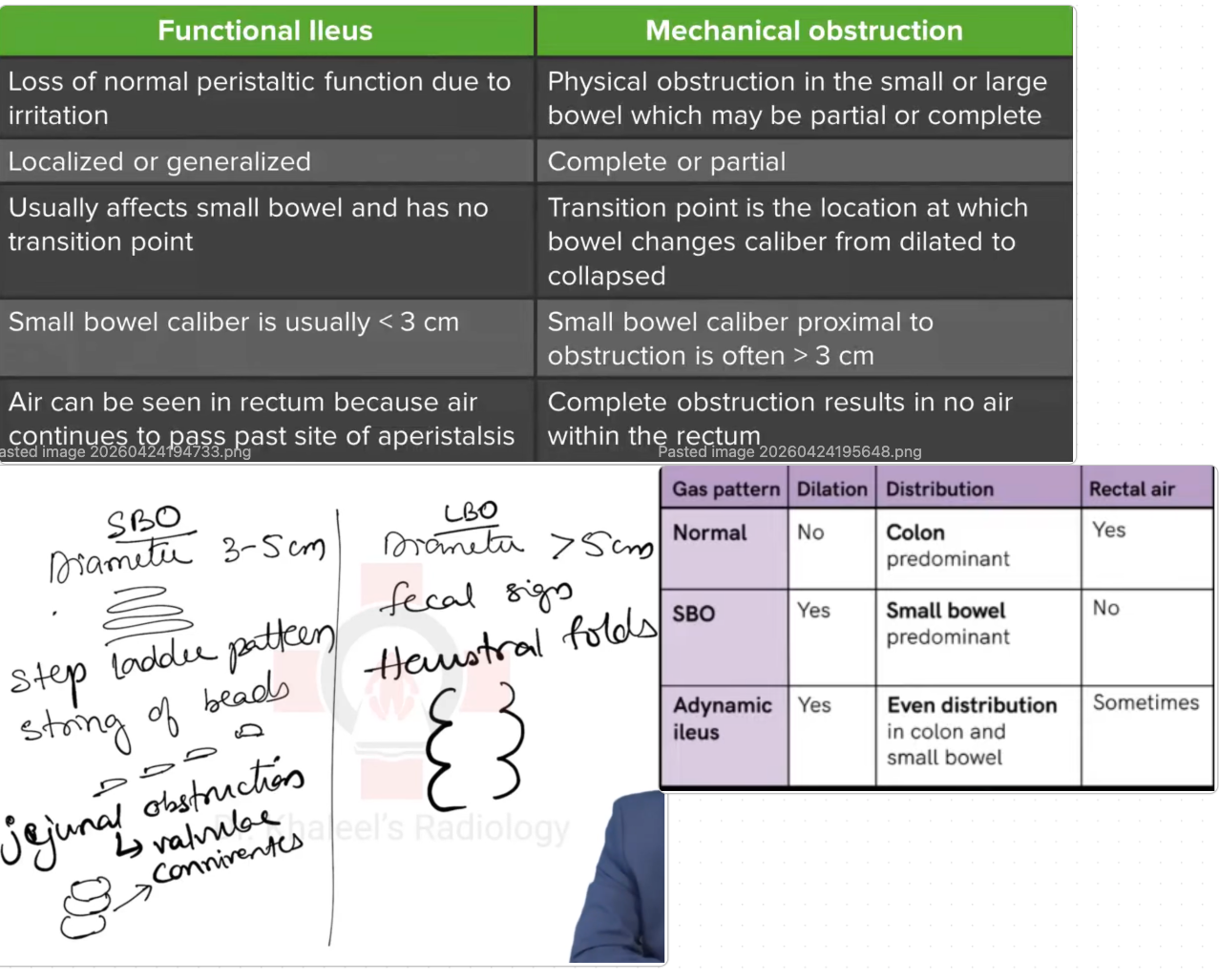
Ileus
Duration:
CC: abdominal distension, nausea/vomiting, poor PO intake
Onset/Progression: s/g-w/i/u
PP: diffuse abdominal discomfort, constipation/no BM or flatus.
PN: denies focal severe colicky pain, peritoneal signs, hematemesis, GI bleed, fever/chills, no hernia symptoms.
mHx: recent surgery/anesthesia, sepsis/infection, opioid use, constipation, prior SBO, hypothyroidism, diabetes,
sHx: tobacco, EtOH, drug use, mobility status, recent hospitalization, baseline bowel habits.
Initial DATA: CBC, CMP/BMP, Mg, Phos; KUB may show diffuse dilation of small + large bowel with gas to rectum; CT if unclear or concern for SBO.
Pending DATA:
MEDS: stop/reduce opioids/anticholinergics,
COURSE:
Plan
Bowel rest: NPO initially or clears if mild/improving
IV fluids + correct dehydration
Replete K/Mg/Phos aggressively
trend KUB
Stop offending meds: opioids, anticholinergics
Early ambulation
Post-op: minimize opioids, gum chewing may help
NG tube if recurrent vomiting / marked distension
Treat sepsis, pneumonia, pancreatitis, etc. if trigger present
CT A/P if concern for transition point / obstruction
Serial abdominal exams + monitor UOP
Escalate / consult Surgery if peritoneal signs, fever/leukocytosis/rising lactate, focal severe pain, progressive distension, no improvement, or SBO cannot be excluded.