Acute respiratory failure with Hypoxia and Hypercarbia
COPD exacerbation
-- days of , S/G Onset, W/U/I Progression and C/I course.
-- ASx +: (dyspnea), Increased purulent cough, Increased sputum production, Fatigue
-- DENIES chest pain, fever/chills, hemoptysis, leg swelling or calf pain, recent travel/immobilization, and orthopnea/PND and sick contact
-- Hx: COPD (Date), last PFT , multiple prior exacerbations with last hospitalization ( *** ), No hx of intubation, smoking,
-- PE: worsening hypoxia or hypercarbia
-- W/U: CBC, BMP,VBG, BNP, Resp Cx, RVP , EKG, CXR, CT?, Echo?
-- MEDS: inhalers _
-- Etiology/DDx: infection, missed home medications, weather, smoke; rule out CHF, PNA, PTX, PE
Plan (COPD add On)
scheduled duonebs q4h / albuterol q2 PRN; space as able,
Prednisone 40mg x5d
PO prednisone 40mg for 5 days; If unable to take PO, give methylprednisolone 40 mg IV daily, then transition to prednisone when able.
CTX 1g IV, Azithromycin 500mg for three days, (Cefepime 2g (5–7 days) if risk of PsA), On DC Augmentin 875/125 mg BID alone to complete ~5 day
Monitoring daily CBC, BMP, tele
Bronchopulmonary hygeine: PEP/flutter
PT/OT for eval
ED/IP/OBG NicWiPP Protocol ADD-ON
consider Pulm consult if refractory or in need of Roflumilast (FEV1 < 50%) or Dupilumab (Eso>300)
O2 prn to maintain SpO2 88-92%
Smoking cessation counseling
NIPPV if resp acidosis, dyspnea, increased WOB; Mechanical ventilation if pH <7.26, PaO2 <55-60 or worsening hypercapnia despite NIPPV
VBG PRN for worsening respiratory status
Discharge with Vitamin D as needed (Vitamin D is given to prevent steroid-related bone loss and address common deficiency in COPD patients)
Meds
Home: Trelegy (ICS [fluticasone] / LABA [vilanterol] / LAMA [umeclidinium])
Inpatient: Dulera (ICS [mometasone] / LABA [formoterol]) + Spiriva (LAMA [tiotropium])
ICU: Budesonide (ICS [budesonide]) + scheduled Duoneb (SABA [albuterol] / SAMA [ipratropium], nebulized).
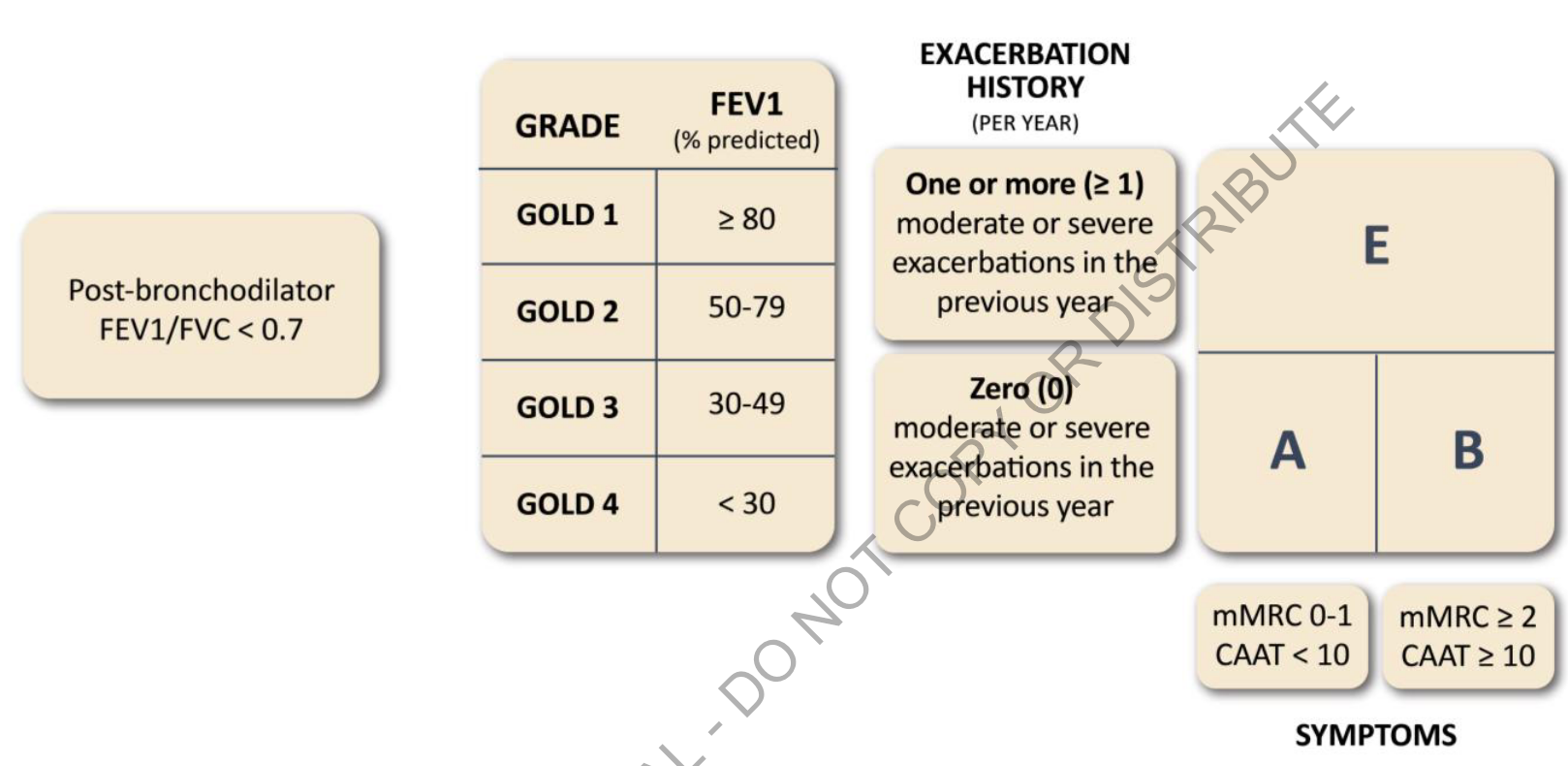
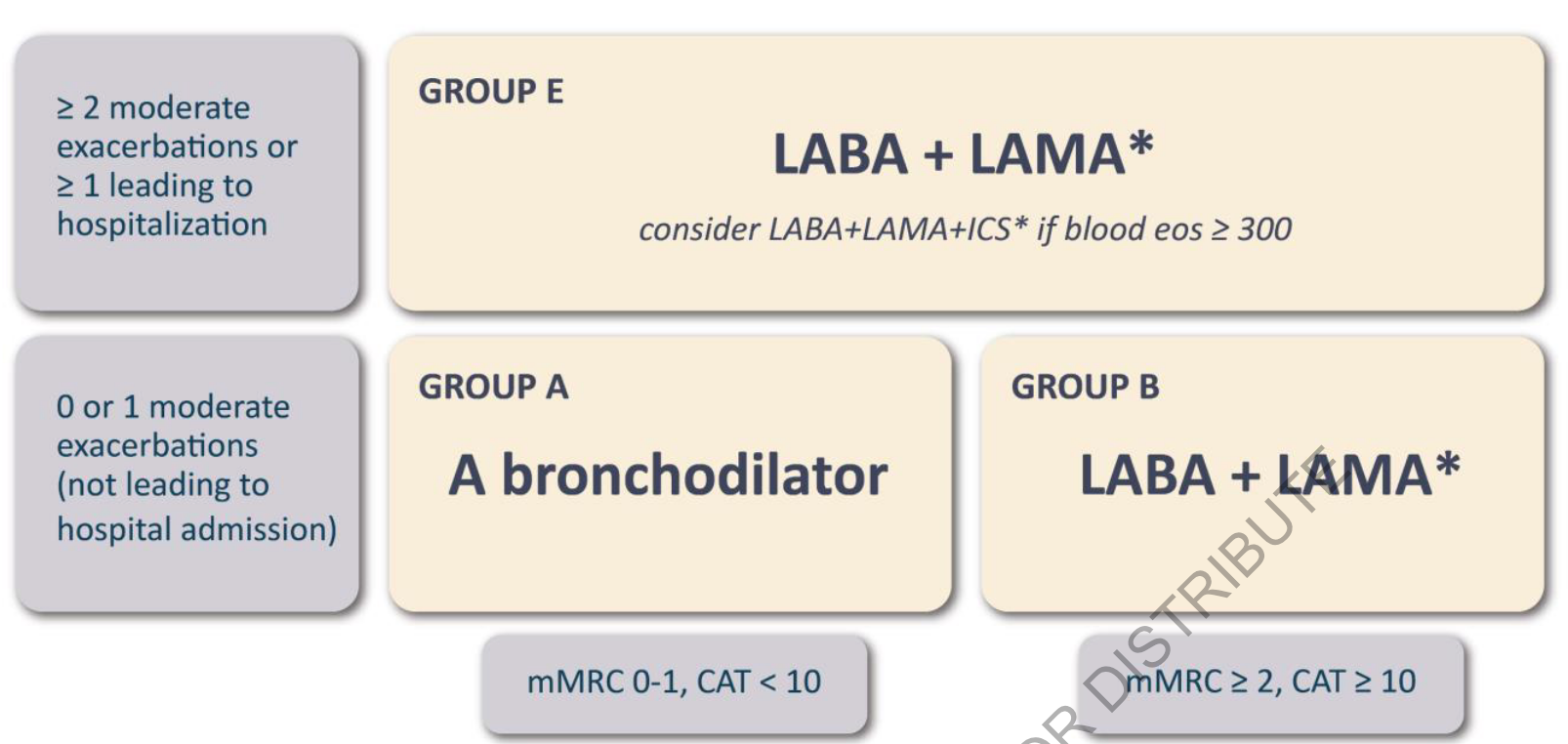
mMRC 0–1 → A
mMRC ≥2 → B
Exacerbations → E